Media centre

- Details
- Details
• Mackay, Queensland
• Windsor Gardens, South Australia
• Hobart, Tasmania
- Details
- Details
- Details
- Details
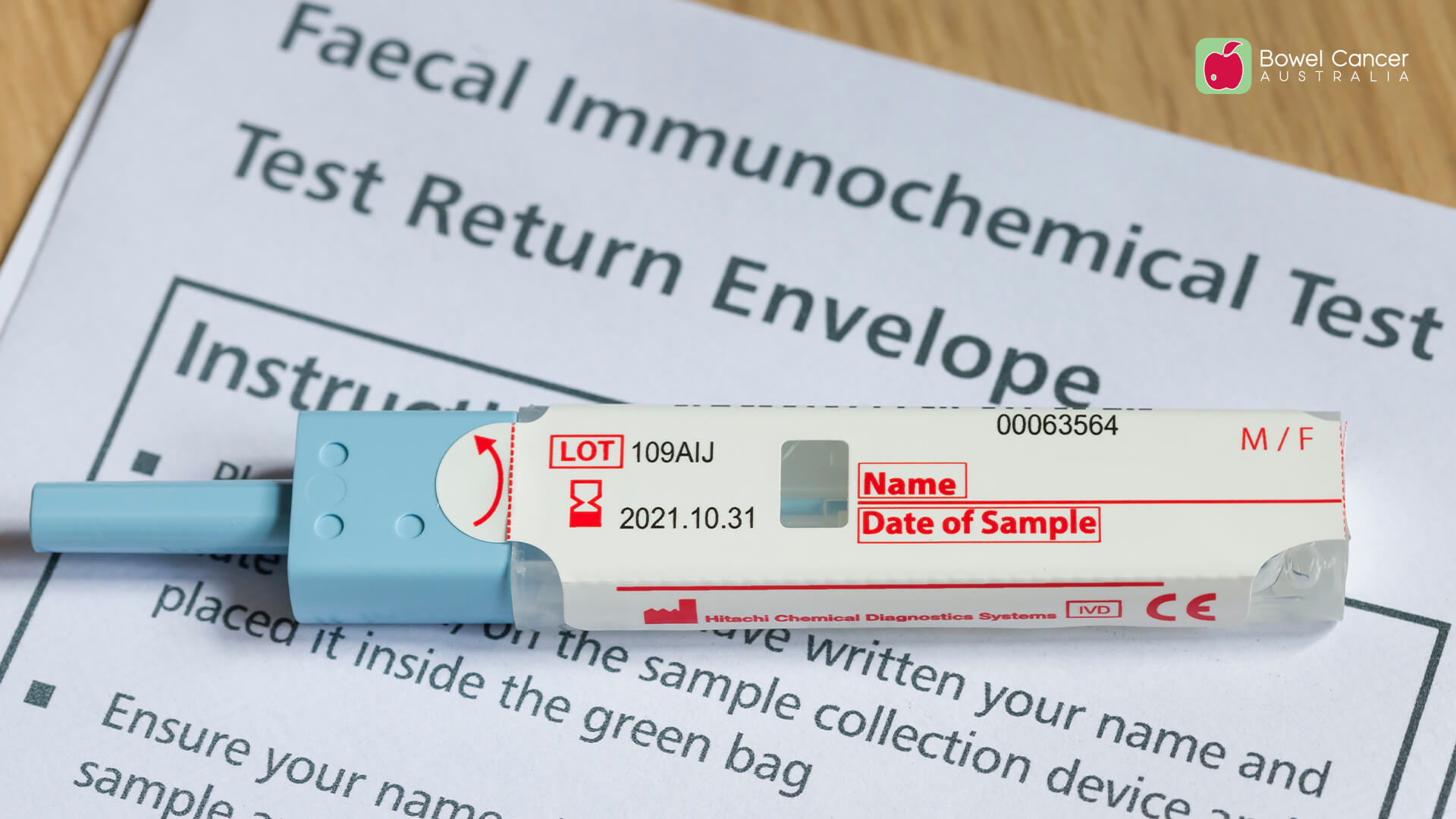
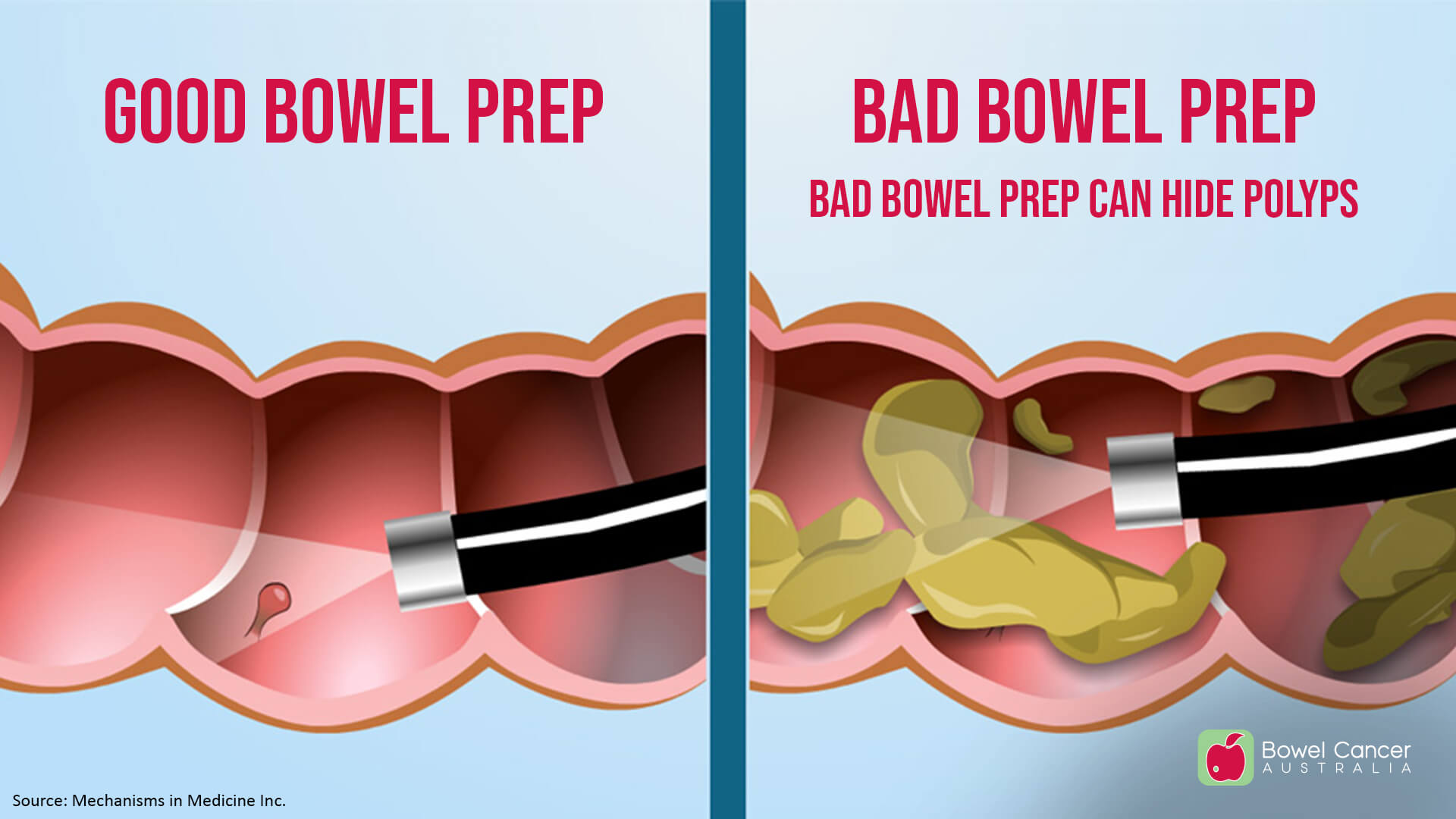
A good bowel prep is essential to a good colonoscopy and critical to detecting bowel cancer or preventing it through the detection and removal of polyps.
In Australia, inadequate bowel prep is observed in around 7% of all colonoscopies. With more than 900,000 colonoscopies performed annually in the country, this can equate to as many as 63,000 inadequate bowel preparations leading to poor or cancelled colonoscopies.
- Details
In a phase 1 trial at Memorial Sloan Kettering Cancer Centre (MSK), published in Nature Medicine, a new vaccine is being investigated as a potential off-the-shelf treatment in bowel and pancreatic cancer patients with a KRAS mutation.
“Having a vaccine that’s ‘off-the-shelf’ would make it easier, faster, and less expensive to treat a larger number of patients,” says gastrointestinal oncologist at MSK, Dr Eileen O’Reilly, who co-led the trial. “This gives hope for people with pancreatic and bowel cancer who have been out of effective treatments when their disease returns.”
- Details
Bowel cancer is the third most diagnosed and second deadliest cancer in Australia, yet people diagnosed with bowel cancer don’t receive the same level of support as those with other common cancers.
In the lead-up to World Cancer Day on Sunday 4 February, Bowel Cancer Australia and Icon Cancer Centre have announced plans to place specialist Bowel Care Nurses in select Icon Cancer Centres across Australia, offering greater support for patients with bowel cancer and helping to close the care gap.
- Details