In February 2023, the Tasmanian Premier announced $38 million in funding to deliver an additional 22,000 endoscopies over the next four years with the aim of driving down waiting lists to a sustainable level of 2,500 people at any one time by June 2027. In August 2021, the Tasmanian Budget delivered additional funding for elective surgery. As part of a $40 million top up, funding for an additional 7,000 elective surgeries was promised, on top of funding committed to at the State Election for an extra 22,300 surgeries and endoscopies. On 9 April 2019, the Opposition Leader Bill Shorten promised to invest $500 million to reduce waiting times for cancer treatment and surgery in public hospitals across Australia if elected. Mr Shorten cited official data, stating 83 per cent of people who received a positive-test result from the government's bowel cancer screening program did not have a follow-up colonoscopy within the recommended time. According to the Premier's media release, 'the Government's $5 million commitment towards additional colonoscopies will see SA Health work with the private sector to carry out an extra 2,700 colonoscopies over the next nine months, the remaining overdue colonoscopies will be funded with Elective Surgery Funds. This is in addition to the approximately 25,000 colonoscopies carried out in the SA public health system each year'.

Tasmania
A Colonoscopy Wait-time and Performance Guarantee

Wait-time and performance guarantee | National healthcare agreement | House of representatives: E-petition | Further developments
Bowel Cancer Australia advocates for a colonoscopy wait-time and performance guarantee:
| A colonoscopy wait-time and performance guarantee
A guarantee - with recording, reporting and resourcing - to address delays in diagnosis
Bowel Cancer Australia is calling on Federal, State and Territory Governments to commit to a national Colonoscopy Wait-time and Performance Guarantee – with recording, reporting and resourcing - to address delays in diagnosing Australia’s second biggest cancer killer.
“It is unacceptable that people with a positive screen or bowel cancer symptoms have to wait six months or longer for a colonoscopy to learn if they have cancer,” said Bowel Cancer Australia Chief Executive, Julien Wiggins.
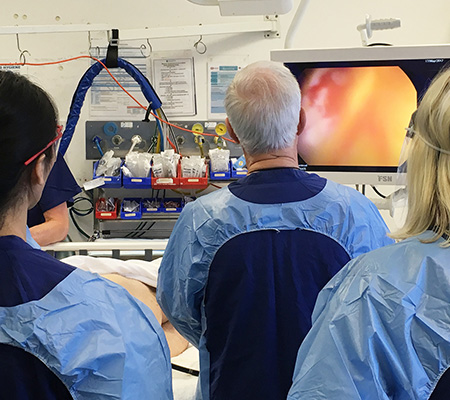
“During a colonoscopy, pre-cancerous polyps can be detected and removed before they develop into something more sinister requiring surgery and treatment,” said colorectal surgeon, Graham Newstead AM.
“If bowel cancer is detected, and it is still in the earliest stages, almost 99% of cases can be successfully treated,” he added.
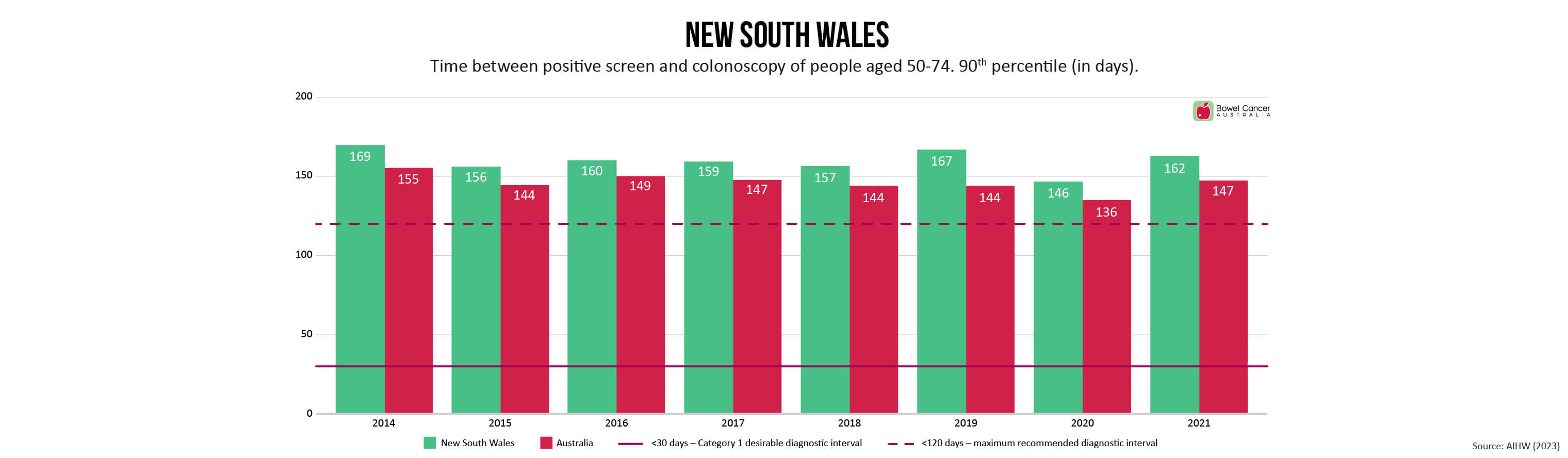
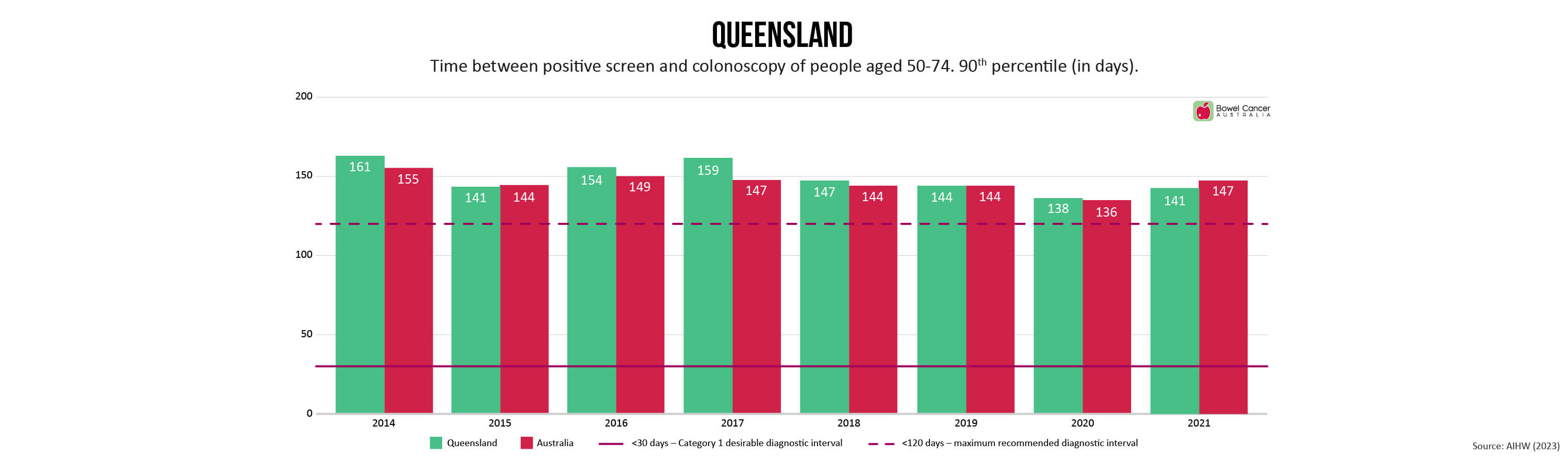
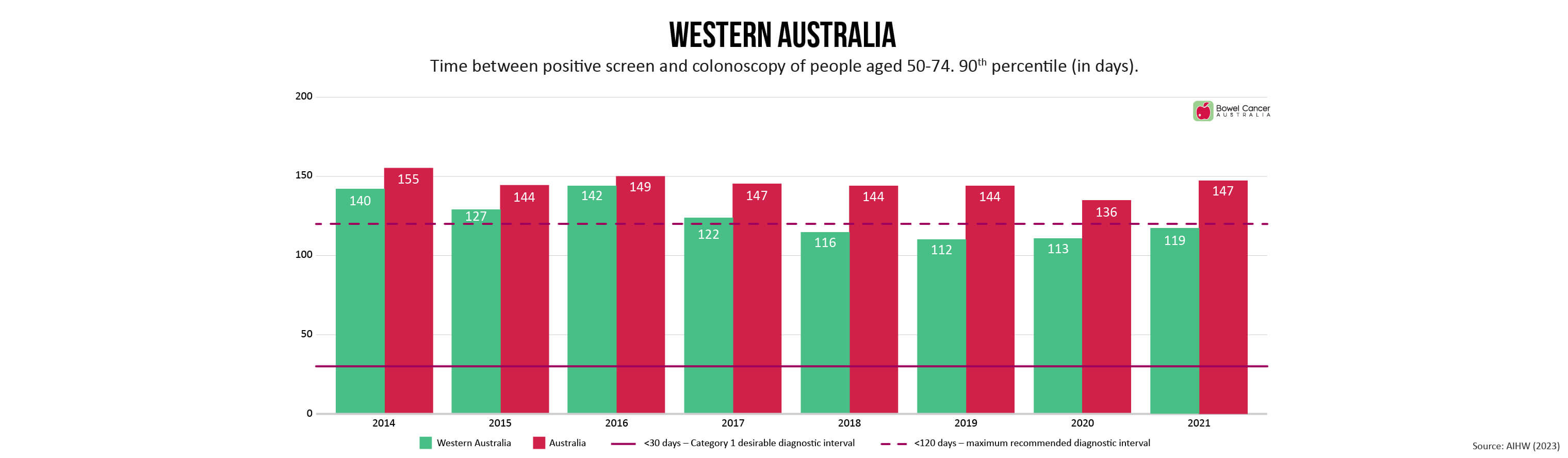
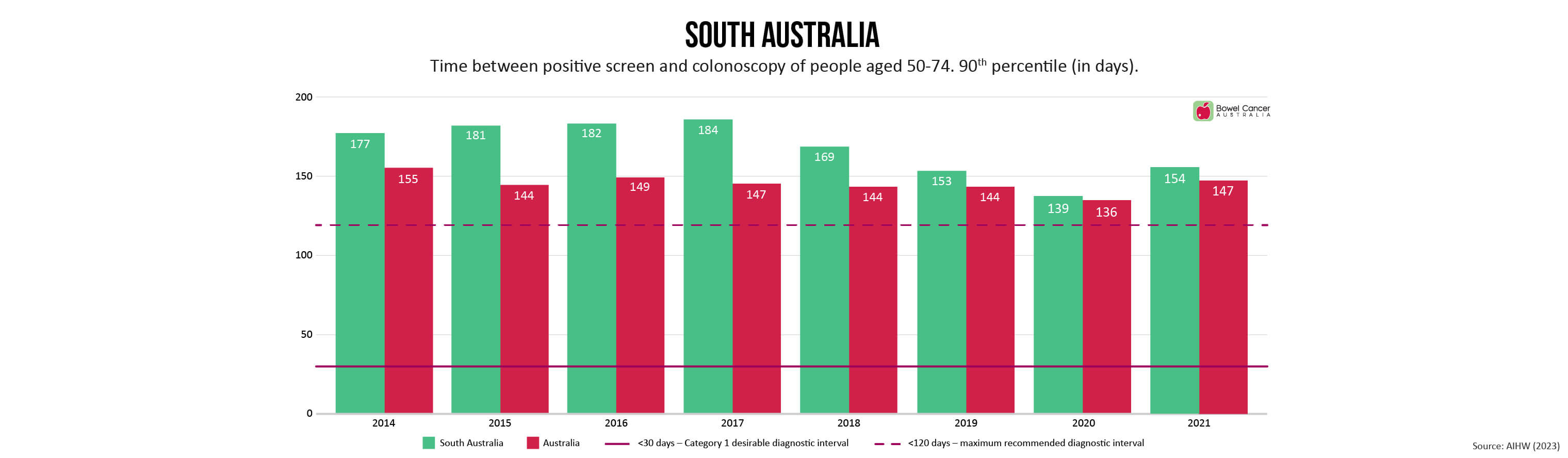
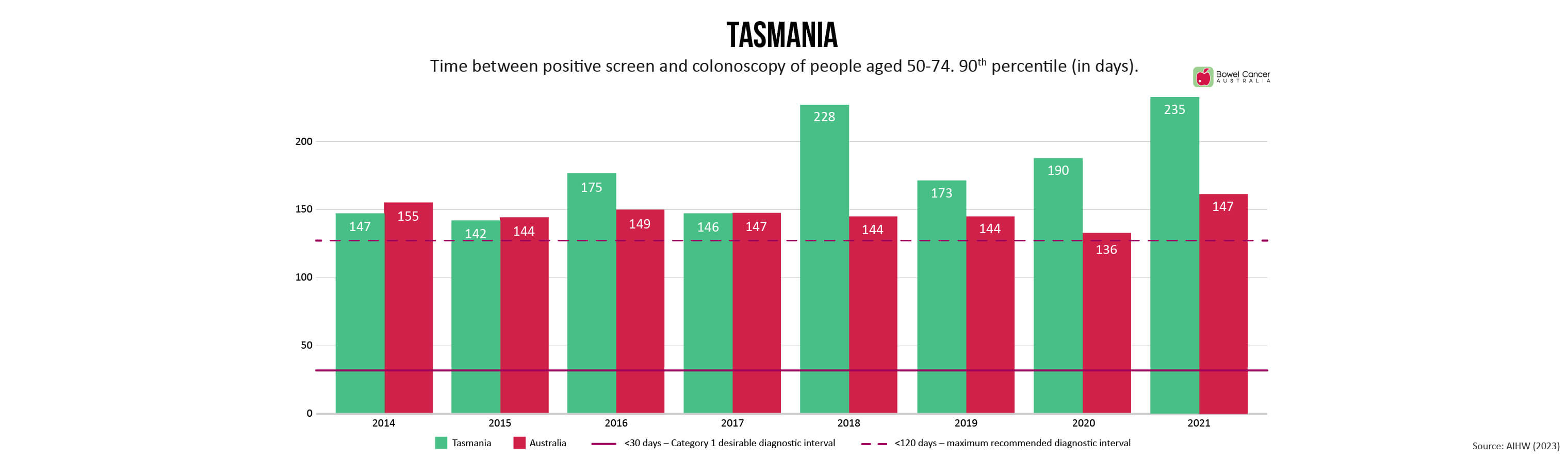
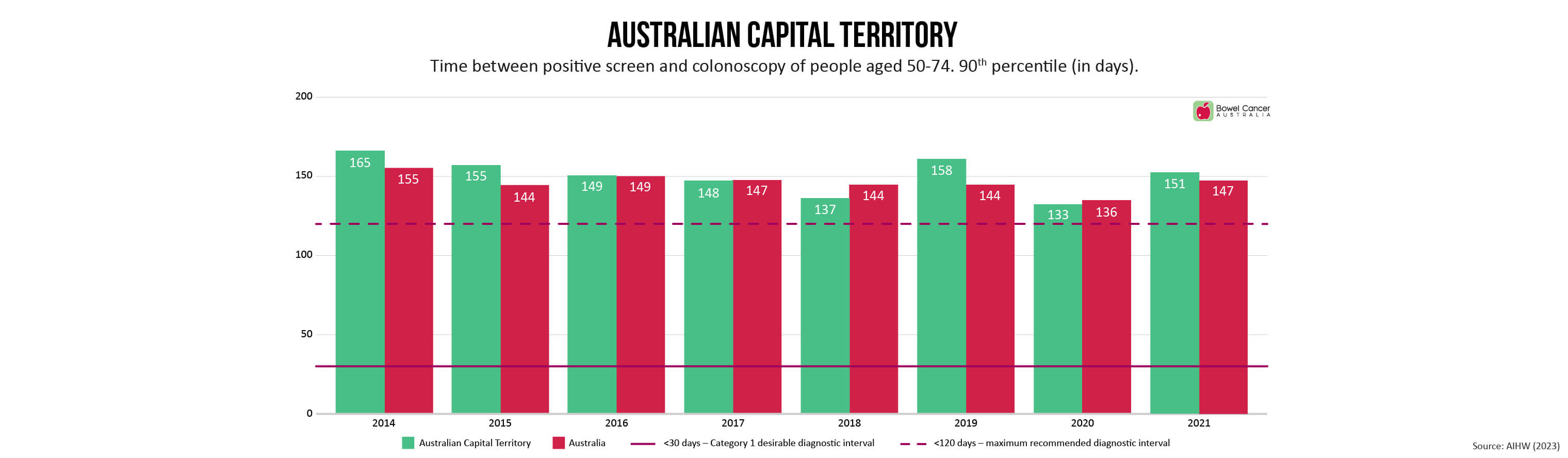
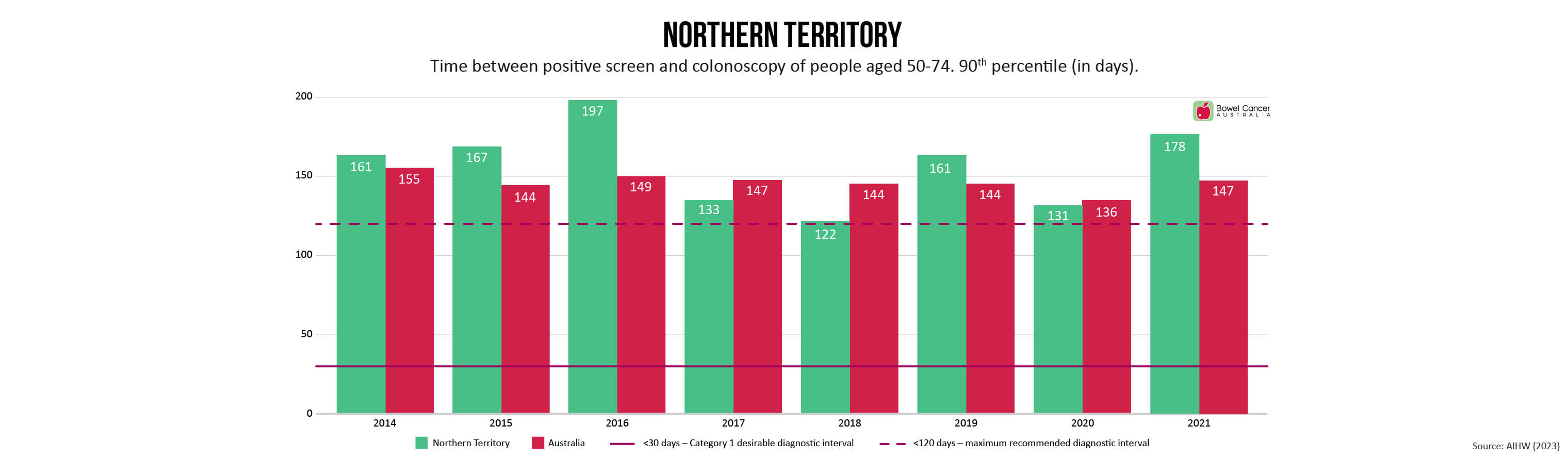
Bowel Cancer Australia has long advocated for referral to colonoscopy within 30 days to minimise patient stress and anxiety, as recommended in the Optimal Care Pathway for people with bowel cancer.
Newly released medical guidelines, however are now recommending patients be referred to colonoscopy within a 120-day threshold.
“Despite extending the recommended timeline-to-diagnosis by 300%, the new timeframes are still not being met,” said Mr Wiggins, who shares concerns expressed by individuals involved in developing the new guidelines, that the extended threshold de-emphasises the need for prompt evaluation.
Research shows diagnostic intervals exceeding 120 days are associated with poorer outcomes, yet the number of days 90% of National Bowel Cancer Screening Program (NBCSP) participants with a positive screen are waiting range between 116-181 days, depending on where they live in the country.
“What is needed is a Colonoscopy Wait-time Guarantee,” said Mr Wiggins, “complete with public wait-time recording, reporting and adequate resourcing of colonoscopy.”
“Publishing wait-times will highlight where resources need to be allocated to improve patient care and will demonstrate a clear commitment on the part of government to meet their own endorsed colonoscopy wait-time recommendations,” said Mr Wiggins.
The National Healthcare Agreement affirms all governments agree that Australia’s health system should, among other things, provide every Australian with timely access to quality health services based on their need, not their ability to pay, regardless of where in Australia they live.
In the lead up to September 2018, the Council of Australian Governments (COAG) is considering a longer-term public hospital funding agreement.
The Agreement will establish a list of commitments which includes public hospital funding, as well as public and private hospital-performance reporting.
The new Agreement commenced on 1 July 2020 – the same year that full implementation of the National Bowel Cancer Screening Program occured and demand for colonoscopies is projected to reach 1.11 million.
In February 2018, Bowel Cancer Australia encouraged Australians to sign the e-petition calling on the House of Representatives to ensure people with bowel cancer symptoms or a positive screen, receive a colonoscopy with a maximum wait time of 120 days, no matter where in Australia they live.
Timely access to a colonoscopy is essential to reduce bowel cancer deaths and minimise distress and anxiety in people experiencing symptoms or those with a positive screen awaiting investigation.
Thank you to everyone who signed the e-petition. The signing deadline has now passed with over 3,500 signatures collected during the 28-day period.
On 10 April 2019, the Prime Minister Scott Morrison announced the Government would invest $34.7 million to reduce waiting times by providing an additional 6,000 surgeries and endoscopies and for primary care support for Tasmanians in rural and remote locations through TazReach.
Nationwide
E-petition
The Colonoscopy Wait-time Guarantee e-petition was presented to the House of Representatives on 21 May 2018 and was referred to the Minister for Health.
The Minister's response stated that the 'Government will work with state and territories to develop an action plan that reflects their respective roles in ensuring capacity can meet the demand for colonoscopy services into the future, beyond the small percentage generated by the National Bowel Cancer Screening Program'.
The response concluded by stating 'while colonoscopy performance measures are not reported at a national level, the AIHW publishes annual monitoring reports against NBCSP key performance indicators, including waiting times and adverse events following colonoscopy. The AIHW will also be tasked with including a 120-day reporting timeframe for waiting times to colonoscopy in future reports'.
2018-19 Federal Budget
The 2018-19 Federal Budget provided $35 million over four years for a national partnership with State and Territory governments to fund the follow-up of people who have received a positive at-home bowel cancer screening test result and are not recorded as having attended a follow-up appointment with a health professional.
Council of Australian Government (COAG) Health Council
The federal, state and territory Health Ministers met in Sydney on 13 April 2018 at the COAG Health Council to discuss a range of national health issues.
Major items discussed by Health Ministers included, among other things, the impact of the National Bowel Cancer Screening Program expansion on colonoscopy demand and waiting times.
A key impact of the Program and its expansion is the increased volume of people requiring diagnostic assessment through colonoscopy.
Health Ministers agreed that the Commonwealth and states and territories should work together to ensure that future infrastructure and workforce capacity and development are better matched to the expected increase in demand.
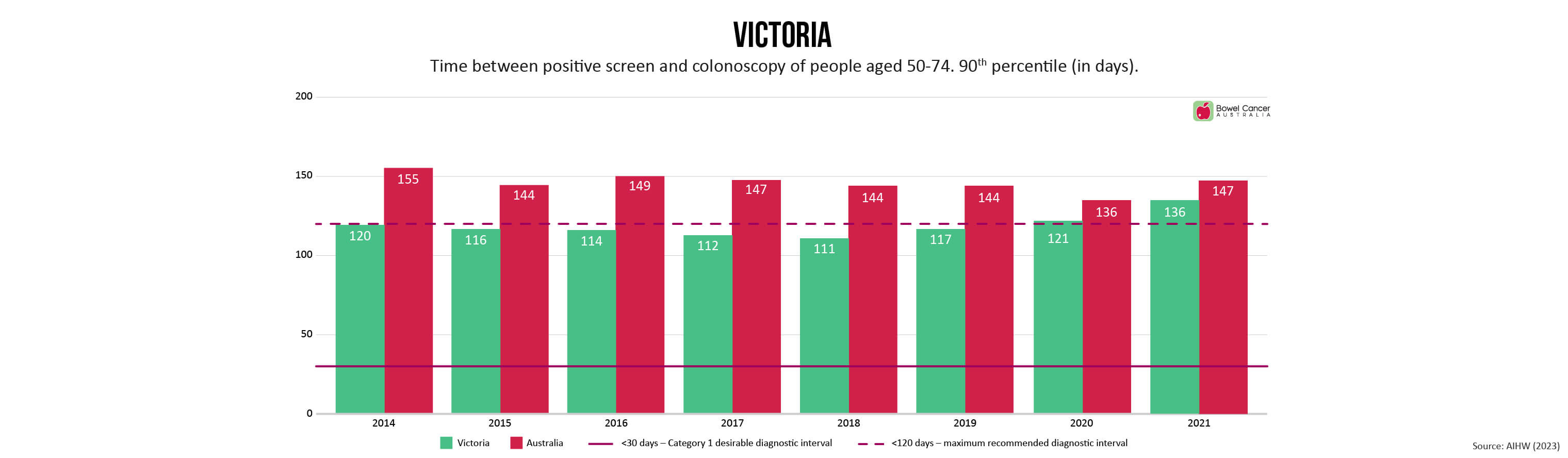
Victoria
On 1 April 2018, the Victorian Labor Government announced a $12 million injection into Victorian hospitals to fast-track access and cut waiting times for colonoscopy procedures.
This will provide colonoscopies for 6,635 patients across Victoria who are in the most urgent category and who have been waiting the longest.
From 1 July 2018, new Colonoscopy Guidelines for Victorian Patients will come into force, with a target to ensure all Victorians patients in urgent need of colonoscopy receive them within 30 days.
According to media reports, the Victorian Government is calling for a united approach to mounting colonoscopy waiting lists. The Victorian Premier wants Canberra to increase infrastructure and the workforce to perform colonoscopies. The Victorian Government is also calling on states to develop uniform reporting to ensure colonoscopies are completed within the 120-day guideline as well as assurances category 1 patients with be seen within 30 days of a referral.
South Australia
The South Australian Government committed $5 million to a Bowel Cancer Prevention Initiative to:
On 31 August 2018, the South Australian Government announced a $45 million investment to significantly reduce the number of overdue elective surgery patients in South Australia, including patients waiting beyond recommended clinical time frames for colonoscopy procedures.
There are around 4,100 South Australians who have been waiting for a colonoscopy beyond recommended clinical time frames.